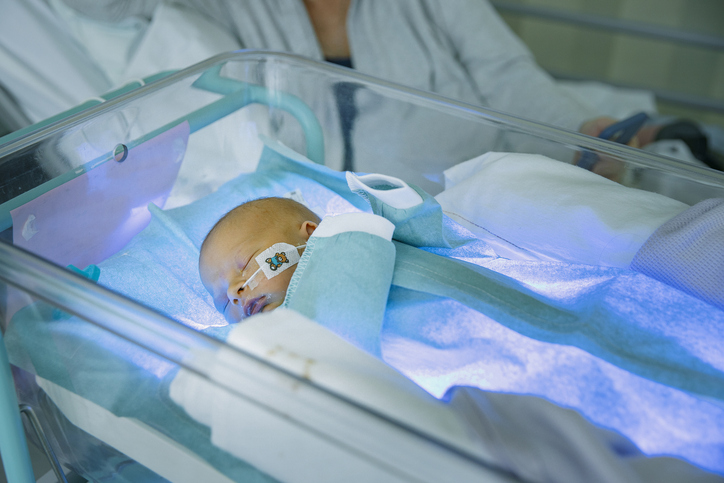
Jaundice is very common in newborns, with approximately 80% of babies showing some signs of jaundice.
While in most cases, jaundice is resolved in the first seven days post-delivery, other cases can require treatment by phototherapy and blood transfusions. Without timely and effective treatment, jaundice can lead to life-threatening complications, especially in newborns affected by hemolytic disease of the fetus and newborn (HDFN), bilirubin levels are higher due to a more significant breakdown of red blood cells.
What is HDFN?
Hemolytic disease of the fetus and newborn (HDFN) is an immune-mediated red blood cell disorder that occurs when a baby’s RBCs break down quickly, which is called hemolysis. HDFN is caused by a mismatch between a mother’s and her baby’s blood type (A, B, AB, or O) or Rhesus (Rh) factor (Rh-positive or Rh-negative) during pregnancy.
What is jaundice?
Also called hyperbilirubinemia, jaundice is the yellowing of the skin and whites of the eyes that occurs as a result of high levels of bilirubin levels in the blood. Bilirubin is produced when red blood cells break down. In babies affected by HDFN, the red blood cells have been attacked by the maternal antibodies, causing them to break down and leading to higher levels of bilirubin than in babies unaffected by HDFN. Following delivery, the placenta no longer filters the bilirubin, causing it to build up in the baby’s blood.
Jaundice commonly presents in newborns and often resolves without treatment within the first seven days. However, if bilirubin levels don’t fall, treatment by phototherapy is required. Phototherapy uses blue light therapy to break down the bilirubin in the baby’s blood so it can be more easily eliminated. If this doesn’t quickly reduce bilirubin levels, blood transfusions or exchange transfusions may be conducted.
What are the long-term risks of jaundice?
If jaundice is not effectively treated, the greatest risk is that the bilirubin will cross the blood-brain barrier. This is known as kernicterus, where bilirubin can damage the brain or central nervous system, causing long-term brain damage, cerebral palsy, learning disabilities, hearing loss, vision problems, dental issues, seizures and sensory problems.
Managing and treating jaundice in HDFN-affected newborns
Early diagnosis of jaundice in newborns affected by HDFN is done by testing the umbilical cord blood shortly after birth. This measures the bilirubin levels before symptoms of jaundice become visible, allowing early medical intervention to reduce the bilirubin in the blood and avoid complications. Regular testing of the bilirubin levels to check whether the levels are increasing or decreasing will guide treatment choices and indicate if treatment is effective.
When the baby’s bilirubin levels have dropped to normal levels and there are no other health issues, discharge from the hospital will be possible. Following up with your doctor is important after discharge to monitor the baby’s bilirubin levels and avoid hospital readmission.