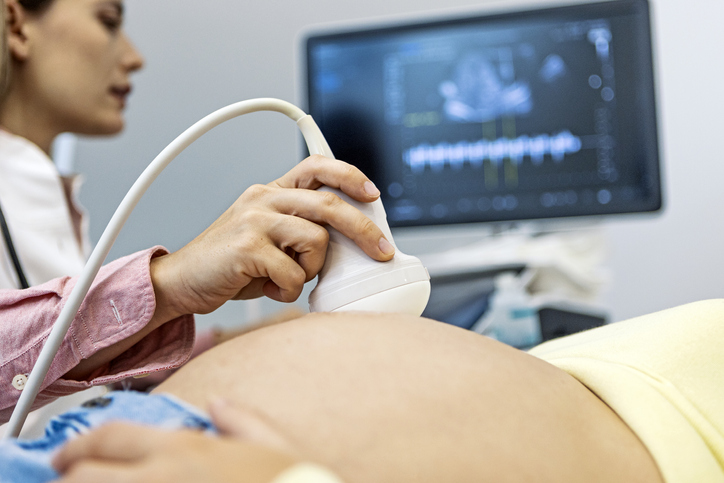
What is HDFN?
Hemolytic disease of the fetus and newborn (HDFN) is a condition that occurs when a baby’s red blood cells (RBCs) break down quickly, which is known as hemolysis. Several tests can be performed prior to the baby’s birth to check for the presence of both HDFN and fetal anemia, which is a common symptom of HDFN.
Fetal anemia is monitored with the use of a noninvasive method known as a middle cerebral artery (MCA) Doppler ultrasound measurement
The basics of HDFN
In HDFN, certain maternal antibodies cross the placenta and reduce the lifespan of fetal RBCs, which causes the development of fetal anemia. The fetus’s RBCs begin to break down at a rapid rate, which is called erythroblastosis fetalis.
HDFN occurs because of a mismatch—incompatibility—between a mother’s and her baby’s blood type (A, B, AB, or O) and/or Rhesus (Rh) factor during pregnancy. The major antigens on human RBCs are the O, A, and B antigens.
RBCs can sometimes have another antigen, which is a protein called the Rh(D) antigen. The RhD antigen is either present or absent on the outside or surface of human RBCs. In Rh-positive individuals, the Rh(D) antigen is present on their RBCs and their blood group is known as RhD- positive. In Rh-negative individuals, the Rh(D) antigen is not present on their RBCs and their blood group is known as RhD-negative.
Read more about HDFN testing and diagnosis
Fetal anemia in HDFN
(MCA) Doppler ultrasounds are performed approximately every two weeks during a pregnancy, for the purposes of stratifying the risk of a fetus. Depending on the doctor, this procedure typically is performed in mothers whose pregnancies have reached 16 to 24 weeks.
MCA Doppler ultrasound is also used when a critical antibody titer has been reached. The titer is based on the mother’s history of prior pregnancies that have been affected by HDFN and fetal anemia.
Predicting fetal anemia with the use of MCA Doppler ultrasound has transformed the evaluation of Rh-sensitized pregnancies.
Why use MCA Doppler ultrasound studies in fetal anemia?
When a fetus develops anemia, an increase in stroke volume and thus a rise in cardiac output can be observed. This situation is associated with the fetus developing a hyperdynamic circulation. In such cases, blood flow becomes redistributed to vital end organs, such as the heart, brain and adrenal glands. Changes in vascular resistance, along with a decrease in blood viscosity, or thickness, are often reported as well.
The value of the Doppler ultrasound in evaluating fetal anemia is based on the idea that as long as the cross-sectional area of a blood vessel stays constant, blood velocity, or rate, is directly proportional to blood flow. In fact, decreased blood viscosity leads to increased blood flow. Such changes can be observed using an MCA Doppler ultrasound.
The MCA is the vessel chosen for Doppler ultrasound assessment because of its sensitivity to the effects of hypoxia, or insufficient amounts of oxygen, and its ease of accessibility.
Current treatment of HDFN
In addition to tests throughout pregnancy and after delivery, there are several treatment methods available for infants with HDFN. One of these is the administration of Rh immunoglobulin (RhIg) to RhD-negative mothers throughout their pregnancy and then shortly following the birth of an RhD-positive baby, which has dramatically decreased the incidence of Rh-hemolytic disease. RhIg is a medication that is administered as an injection. This medicine can prevent severe fetal anemia from occurring in future pregnancies.
RhIg therapy cannot help if an Rh-negative mother has already made antibodies. In such instances, the fetus will need to be checked throughout the pregnancy, usually with the use of an ultrasound.