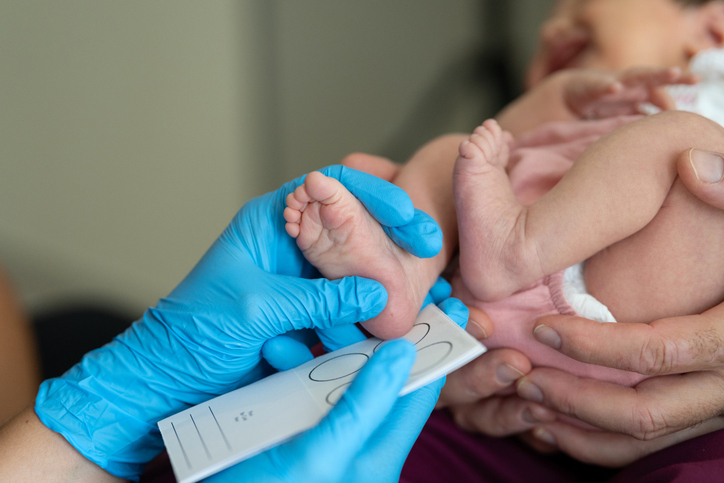
Newborns with hemolytic disease of the fetus and newborn (HDFN) are often born prematurely and require close monitoring and specialist care for the first days or weeks following delivery, often in the neonatal intensive care unit (NICU).
Following discharge, a baby affected by HDFN will continue to need regular checkups, but it can be difficult to determine the right time to bring your baby in for a follow-up appointment.
What is HDFN?
Hemolytic disease of the fetus and newborn (HDFN) is an immune-mediated red blood cell (RBC) disorder that occurs when a baby’s RBCs break down quickly, which is called hemolysis. HDFN is caused by a mismatch between a mother’s and her baby’s blood type (A, B, AB, or O) or Rhesus (Rh) factor (Rh-positive or Rh-negative) during pregnancy. Numerous antibodies to RBC antigens can be linked to HDFN, such as those from the ABO and Rh blood group systems.
How long will my HDFN baby have to stay in the hospital?
The length of your baby’s hospital stay will depend on the severity of their symptoms and their gestational age at birth. If no complications develop and your baby responds well to treatment for jaundice and anemia, you will be able to take your baby home sooner, once he or she reaches certain milestones.
As well as passing HDFN-related tests, these milestones include a hearing test, a pulse oximetry test to check the oxygen level in the blood and a newborn blood screen test.
Before being discharged, the NICU medical team will test your baby’s blood to measure the bilirubin levels. If they have fallen to a safe level, your baby will be able to leave the hospital. You may still need to continue phototherapy treatment at home, with the help of a special phototherapy blanket.
Follow-up appointments after initial discharge
Once you and your baby have been discharged from the hospital, you will need to settle into your own daily routine. Your NICU healthcare team will give you a clear idea of when to schedule your first follow-up appointment, but it is usually within the first days or week following discharge.
These follow-up sessions will include monitoring for late-onset anemia, which can develop between two and 12 weeks of life. Your baby’s bilirubin levels will continue to be measured to check for jaundice flare-ups. In addition, your baby’s health, nutrition and development will be evaluated on a regular basis.
When to seek immediate medical attention
While most infants with HDFN will recover normally, you should watch your infant closely for any signs of anemia or jaundice. If these suddenly appear or worsen, you may want to consider taking your baby to your preferred hospital’s emergency department immediately, as a baby’s health can change rapidly.
Longer-term considerations for HDFN infants
HDFN is not usually associated with long-term complications except in rare severe cases. The antibodies that attack red blood cells of a baby affected by HDFN are generally eliminated in the first eight to 12 weeks of life. If anemia and jaundice are successfully treated, your baby will not have any lasting effects. In some cases, babies may need top-up transfusions post-discharge in the first months, including once discharged from hospital.